Hair thinning can appear slowly, yet its impact feels immediate. For many people, seeing more hair fall than usual raises concern about overall health. Understanding the medical reasons behind hair loss helps identify effective ways to manage it and support new growth.
This article explores the most common medical causes that lead to thinning hair and how each one can be treated. It looks at how genetics, hormones, nutrition, immune health, and medications affect hair strength and growth. By learning what drives the problem, anyone can take informed steps toward improving hair health and preventing further loss.
Androgenetic Alopecia: Genetic hair thinning treated with minoxidil or finasteride

Androgenetic alopecia is the most common cause of gradual hair thinning in both men and women. It often passes through families and tends to follow a predictable pattern. Men may notice recession at the hairline or crown, while women usually see diffuse thinning across the scalp.
This condition develops from a sensitivity of hair follicles to androgens. Over time, affected follicles shrink and produce finer hair. Treatments such as minoxidil and finasteride can slow progression and may encourage regrowth, but results vary between individuals.
Some people also add a hair loss shampoo for men or women to support scalp health and reduce shedding. Dermatologists often recommend combining topical or oral therapy with proper scalp care to maintain the best long-term outcomes.
Telogen Effluvium: Hair shedding from stress or illness; managed by addressing underlying causes

Telogen effluvium causes sudden, diffuse hair shedding that often appears a few months after a major stress event or illness. The condition happens when many hair follicles move early into the resting phase, leading to increased daily hair loss.
Common triggers include high fever, surgery, childbirth, medications, or significant emotional stress. Individuals may notice more hair on pillows, in drains, or on brushes. However, the scalp usually looks healthy without scarring or patches.
Most cases improve once the cause is identified and treated. Reducing stress, correcting nutritional gaps, and restoring good overall health help hair recover. In many situations, normal growth resumes within several months.
Nutritional Deficiencies: Lack of iron or biotin mitigated with dietary supplements

Low iron or biotin levels often link to hair thinning. Iron helps red blood cells deliver oxygen to hair roots, while biotin supports healthy keratin formation. Without enough of these nutrients, hair may grow weaker and shed faster.
Women with heavy menstrual cycles or low dietary intake face a higher risk of iron deficiency. In these cases, eating lean meat, beans, or leafy greens can help restore levels. A doctor may also suggest iron supplements to correct the shortage.
Biotin deficiency can occur after restrictive diets or certain health conditions. Eggs, nuts, and whole grains provide natural sources of biotin. For those still lacking, biotin supplements offer a safe way to fill the gap, but testing and medical advice help avoid excess use.
Thyroid Disorders: Hypothyroidism or hyperthyroidism linked to thinning, treated with hormone regulation
Thyroid disorders often affect hair growth because the thyroid gland controls hormone balance. Both hypothyroidism and hyperthyroidism can slow or speed up hair growth cycles, causing strands to fall out faster than they grow. The hair may become dry, brittle, or noticeably thinner across the scalp.
Hypothyroidism results from too little thyroid hormone, while hyperthyroidism comes from too much. Each condition disrupts normal metabolism, which influences how hair follicles function. As a result, hair loss can appear gradually and may accompany other body changes like fatigue or weight shifts.
Doctors usually order blood tests to measure thyroid hormone levels. Treatment focuses on restoring balance
through hormone replacement or medication that limits excess hormone production. Correcting the imbalance often helps improve hair thickness over time.
Autoimmune Alopecia Areata: Immune system attacks follicles; treated with corticosteroids
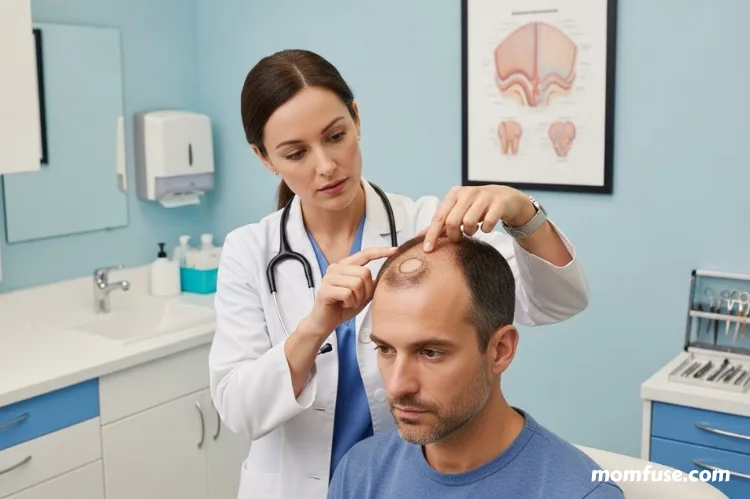
Alopecia areata occurs when the immune system mistakenly attacks hair follicles. This reaction leads to sudden hair loss in small round patches on the scalp or other parts of the body. The condition can appear at any age and often follows periods of stress or illness.
Researchers believe genetic and immune factors both influence its development. The follicles remain alive, so hair can regrow once immune activity calms. However, the pattern and timing of regrowth vary widely from person to person.
Doctors often use corticosteroids to suppress the immune response and reduce inflammation around affected follicles. These may be given through topical creams, injections, or oral medication. In some cases, light therapy or newer immune-targeting treatments may also help control patchy hair loss.
Scalp Infections: Fungal infections like ringworm needing antifungal treatments
Fungal scalp infections can cause patchy hair loss, itching, and flaking. One common type is ringworm of the scalp, also called tinea capitis. It spreads through contact with contaminated objects like hats, brushes, or towels.
Doctors diagnose this infection by examining the scalp and sometimes testing hair samples. Because the fungus grows deep inside hair follicles, topical creams alone rarely work.
Treatment usually includes an oral antifungal medicine such as griseofulvin or terbinafine taken for several weeks. Antifungal shampoos may also help lower the risk of spreading the infection to others.
Good scalp hygiene and avoiding shared personal items can reduce future outbreaks. Early treatment helps stop further hair loss and encourages healthy regrowth once the infection clears.
Medication Side Effects: Hair loss from drugs like chemotherapy, often reversible after stopping treatment

Some medications can interrupt the normal hair growth cycle and cause noticeable thinning. Chemotherapy drugs often lead to sudden hair loss because they target fast-growing cells, including those in hair follicles. Other drugs, such as antidepressants, blood pressure medicines, and hormonal treatments, can also affect hair growth.
In many cases, hair begins to grow back once the medication stops or the dosage changes. The recovery rate depends on the person’s health and type of drug used. New hairs may have a slightly different texture or color at first, but they usually regain normal appearance over time.
Doctors may suggest gentle scalp care, nutrient-rich diets, or prescription treatments to support regrowth. Patients should always talk with a healthcare provider before making medication changes.
Conclusion
Hair thinning often develops due to a mix of medical factors such as hormonal shifts, nutrient deficits, and autoimmune conditions. Each cause may need a different type of care, but early attention usually leads to better outcomes.
Simple changes can make a difference. Balanced meals, gentle hair care, and regular checkups may reduce further loss and support healthier growth. If hair continues to thin, a doctor can identify if the reason stems from thyroid issues, iron deficiency, or other disorders.
Addressing the source of the problem, not just the symptom, remains the most effective way forward. With the right information and proper medical help, individuals can protect hair health and restore confidence in everyday life.
Read Next: Pregnancy Hair Care Tips for Healthier Postpartum Hair
Jessica Fuqua is a mom of two who writes about the messy, beautiful reality of raising kids. She believes parenting advice should feel like a conversation with a friend, not a lecture. When she’s not writing, she’s probably reheating the same cup of coffee for the third time.

